Pancreatic cancer is a complex and often deadly disease that affects the pancreas, an organ essential for digestion and blood sugar regulation. Understanding pancreatic cancer, its risk factors, and treatment approaches is vital for early detection and better patient outcomes. This article will delve into these aspects, providing you with comprehensive insights on the disease, its risk factors, and the available treatment options.
What Is Pancreatic Cancer?
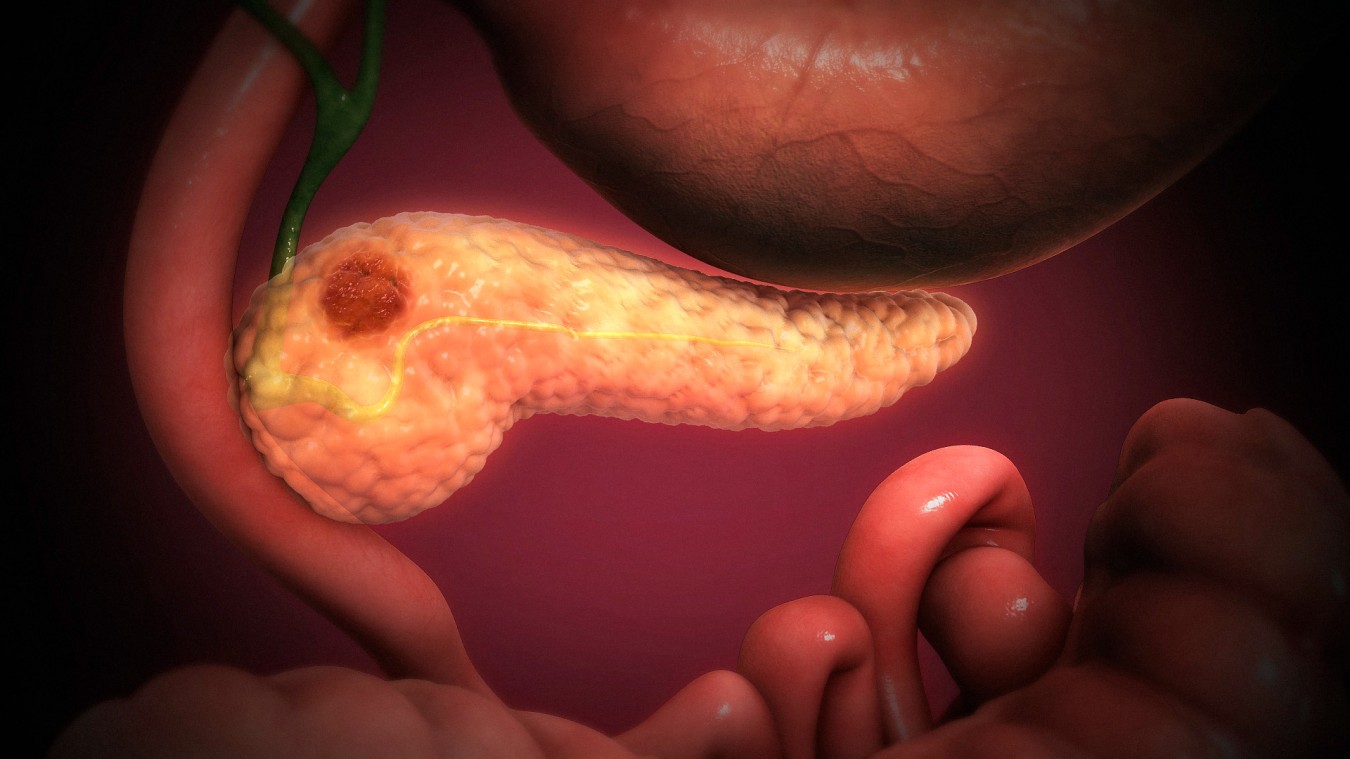
Pancreatic cancer originates in the tissues of the pancreas, which plays a crucial role in digestion and controlling blood sugar levels. The pancreas is located behind the stomach and has two key functions: producing digestive enzymes and regulating blood sugar through insulin production. Pancreatic cancer occurs when abnormal cells in the pancreas grow uncontrollably, leading to the formation of a tumor. Pancreatic cancer is known for its silent nature in the early stages, which makes it one of the most challenging cancers to diagnose.
The Risk Factors of Pancreatic Cancer
Several risk factors contribute to the development of pancreatic cancer. These factors may increase the likelihood of a person developing the disease, though they do not guarantee it. Below are the most common risk factors associated with pancreatic cancer:
1. Age
As with many types of cancer, the risk of pancreatic cancer increases with age. The majority of people diagnosed with pancreatic cancer are over 65 years old, with the risk steadily rising as individuals age.
2. Smoking
Smoking is one of the most significant risk factors for pancreatic cancer. Studies have shown that smokers are two to three times more likely to develop pancreatic cancer than non-smokers. The harmful chemicals in tobacco can cause genetic mutations in the cells of the pancreas.
3. Family History
A family history of pancreatic cancer can increase the risk of developing the disease. If a close relative, such as a parent or sibling, has had pancreatic cancer, you may be at a higher risk. Genetic mutations and inherited conditions can contribute to this increased risk.
4. Chronic Pancreatitis
Chronic inflammation of the pancreas, known as chronic pancreatitis, can increase the risk of developing pancreatic cancer. Long-term damage to the pancreas from inflammation may lead to the development of cancerous cells.
5. Diabetes
People with diabetes, particularly those who develop it after the age of 50, may have an increased risk of pancreatic cancer. The relationship between diabetes and pancreatic cancer is not fully understood, but it is thought that long-standing diabetes can damage the pancreas, increasing the likelihood of cancer development.
6. Obesity
Obesity has been linked to a higher risk of pancreatic cancer. Excess body fat can lead to insulin resistance and inflammation, both of which may contribute to the development of cancer in the pancreas.
7. Genetic Mutations
Certain genetic mutations can increase the risk of pancreatic cancer. Conditions such as hereditary breast and ovarian cancer syndrome, Lynch syndrome, and familial atypical multiple mole melanoma syndrome are known to be linked to a higher risk of pancreatic cancer.
8. Exposure to Chemicals
Exposure to certain chemicals, particularly those used in the dry cleaning and metalworking industries, may increase the risk of developing pancreatic cancer. These chemicals can enter the body through the skin or inhalation and potentially lead to cancerous changes in pancreatic cells.
Symptoms of Pancreatic Cancer
In its early stages, pancreatic cancer often goes unnoticed because it typically does not show clear signs. However, as the cancer grows, it can cause the following symptoms:
- Abdominal pain, which may radiate to the back
- Jaundice (yellowing of the skin and eyes)
- Unexplained weight loss
- Loss of appetite
- Digestive problems, including nausea and vomiting
- Dark urine and light-colored stools
- Fatigue and weakness
If you experience any of these symptoms, especially if they persist, it is important to consult a healthcare professional for further evaluation.
Treatment Approaches for Pancreatic Cancer
Treatment for pancreatic cancer depends on the stage of the disease, the patient's overall health, and other factors. The primary treatment options for pancreatic cancer include surgery, chemotherapy, radiation therapy, and targeted therapies. Let's explore each approach in more detail.
1. Surgery
Surgery is the most effective treatment for pancreatic cancer, but it is only possible if the cancer is detected early and is localized to the pancreas. The two main types of surgery for pancreatic cancer are:
- Whipple procedure (pancreaticoduodenectomy): This surgery involves removing the head of the pancreas, the gallbladder, part of the small intestine, and nearby lymph nodes. It is the most common surgery for pancreatic cancer.
- Distal pancreatectomy: In this procedure, the tail and body of the pancreas are removed, along with part of the spleen.
Surgery may not be an option for patients with advanced pancreatic cancer, as the tumor may have spread to other organs.
2. Chemotherapy
Chemotherapy uses powerful drugs to kill cancer cells or stop their growth. It is often used in combination with other treatments like surgery or radiation therapy. Chemotherapy can be used to shrink the tumor before surgery or to kill any remaining cancer cells after surgery. It may also be used as a palliative treatment to relieve symptoms and improve the patient's quality of life.
3. Radiation Therapy
Radiation therapy uses high-energy rays to kill cancer cells or shrink tumors. It is often used in combination with chemotherapy for patients with locally advanced pancreatic cancer. In some cases, radiation therapy may be used to relieve pain or bleeding caused by the tumor.
4. Targeted Therapy
Targeted therapies are a newer approach to treating pancreatic cancer. These therapies target specific molecules involved in the growth and spread of cancer cells. By blocking these molecules, targeted therapies can stop or slow the growth of the tumor while minimizing damage to healthy tissue.
5. Immunotherapy
Immunotherapy is a treatment that boosts the body's immune system to fight cancer. While still under research, immunotherapy shows promise in treating certain types of pancreatic cancer. Clinical trials are ongoing to determine its effectiveness and safety.
6. Palliative Care
For patients with advanced pancreatic cancer, palliative care is often used to improve quality of life and manage symptoms. Palliative care includes pain management, nutritional support, and emotional care to help patients cope with the challenges of their illness.
Prevention of Pancreatic Cancer
While it is not always possible to prevent pancreatic cancer, there are steps you can take to reduce your risk:
- Avoid smoking and limit alcohol consumption.
- Maintain a healthy weight through regular exercise and a balanced diet.
- Manage chronic conditions like diabetes and pancreatitis.
- Consider genetic counseling if you have a family history of pancreatic cancer.
Understanding pancreatic cancer, its risk factors, symptoms, and treatment approaches is essential for both prevention and early detection. Although pancreatic cancer is a challenging disease, advancements in treatments such as surgery, chemotherapy, radiation therapy, and targeted therapies offer hope for patients. By being aware of the risk factors and staying informed about available treatment options, individuals can take proactive steps toward better health outcomes. If you or a loved one are experiencing symptoms or are at risk, it is crucial to consult a healthcare professional for proper evaluation and care.




