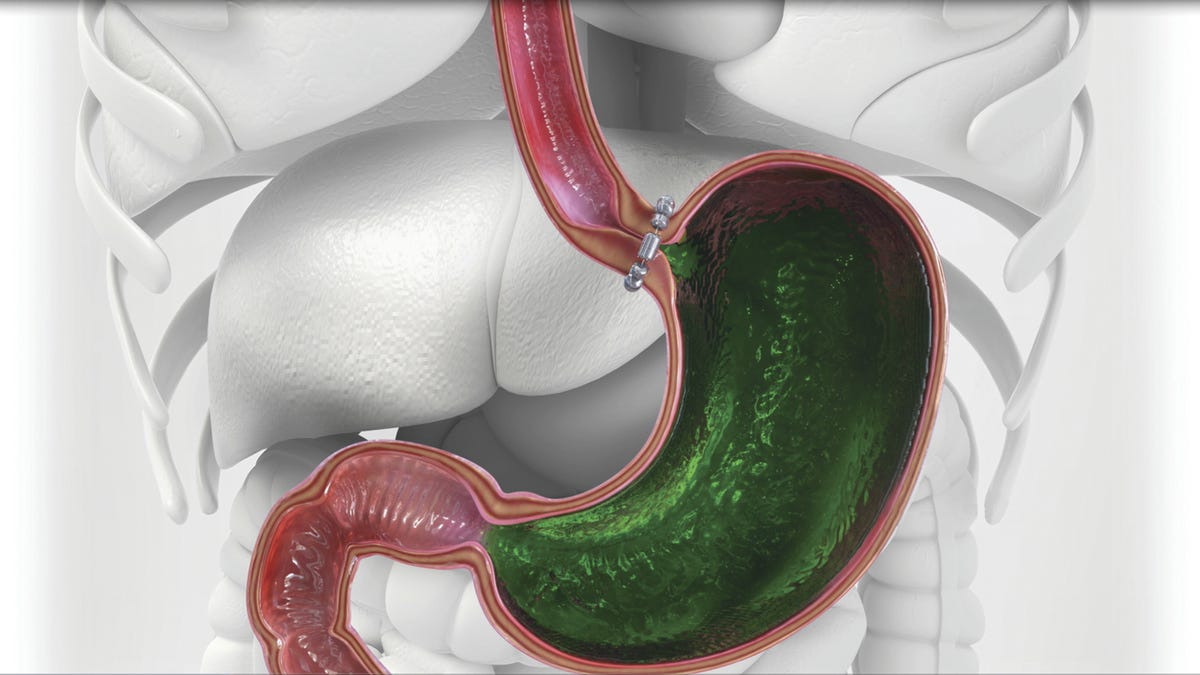
Gastroesophageal reflux disease (GERD) occurs when stomach acid frequently flows back into the esophagus, causing irritation. This chronic condition can lead to symptoms such as heartburn, regurgitation, chest pain, difficulty swallowing, and chronic cough. If left untreated, GERD may cause complications, including esophagitis, Barrett's esophagus, and an increased risk of esophageal cancer.
Common Symptoms of Reflux Disease
- Persistent heartburn
- Acid regurgitation
- Difficulty swallowing (dysphagia)
- Chronic cough or hoarseness
- Feeling of a lump in the throat
- Worsening symptoms after eating or lying down
Why Endoscopic Fundoplication?
Traditional GERD treatments include lifestyle changes, medications, and surgery. However, for individuals who do not respond well to medications or prefer a less invasive option than surgery, endoscopic fundoplication offers a minimally invasive, effective, and durable solution.
Advantages of Endoscopic Fundoplication
- Minimally invasive procedure (no external incisions)
- Faster recovery time compared to traditional surgery
- Reduction in dependency on acid-reducing medications
- Lower risk of complications
- Improved quality of life
Who Is a Candidate for Endoscopic Fundoplication?
Not every GERD patient is an ideal candidate for this procedure. The best candidates are individuals who:
- Have chronic acid reflux symptoms despite medication use.
- Experience frequent regurgitation or nighttime reflux.
- Prefer a less invasive alternative to traditional fundoplication surgery.
- Have been diagnosed with small hiatal hernias (less than 2 cm).
- Want to reduce long-term dependence on proton pump inhibitors (PPIs).
Patients with severe esophageal motility disorders, large hiatal hernias, or Barrett’s esophagus may need alternative treatment options.
How is Endoscopic Fundoplication Performed?
Endoscopic fundoplication is performed using a flexible endoscope inserted through the mouth into the stomach. The procedure typically involves:
- Preparation: The patient is sedated to ensure comfort.
- Endoscopic Insertion: A specialized endoscope is guided down the esophagus.
- Tissue Folding and Fastening: Using an advanced suturing or stapling device, the upper part of the stomach (fundus) is folded around the lower esophagus, reinforcing the lower esophageal sphincter (LES).
- Closure and Recovery: The procedure is completed within 45-60 minutes, and the patient is monitored for a few hours before being discharged.
How Successful is Endoscopic Fundoplication?
Clinical studies have shown that endoscopic fundoplication significantly reduces GERD symptoms and improves quality of life. Success rates vary based on patient selection and technique, but key findings include:
- 80-90% of patients experience symptom relief within the first few months.
- Many patients reduce or eliminate their need for acid-reducing medications.
- Durable symptom control has been observed in long-term follow-ups.
- Fewer complications compared to traditional surgical fundoplication.
Factors Affecting Success Rates
- Severity of GERD before treatment
- Adherence to post-procedure dietary guidelines
- Presence of hiatal hernia
- Individual healing response
Conclusion
Endoscopic fundoplication is an effective, minimally invasive treatment for GERD, offering long-term symptom relief and reducing medication dependence. It is an ideal option for patients seeking an alternative to traditional surgery. If you suffer from chronic reflux and want to explore advanced treatment options, consulting a general surgery specialist in Cyprus can help determine if endoscopic fundoplication is right for you.




